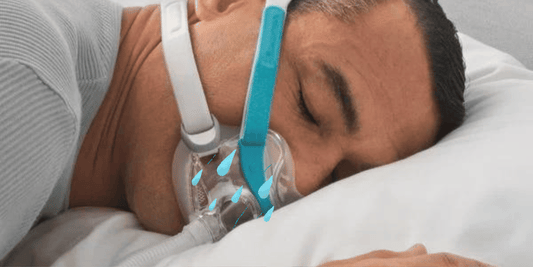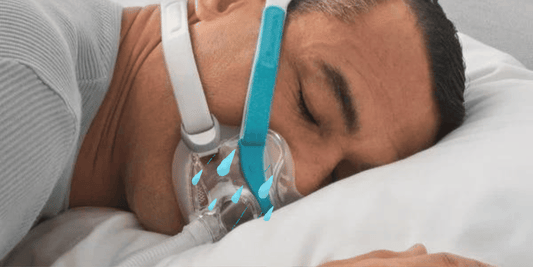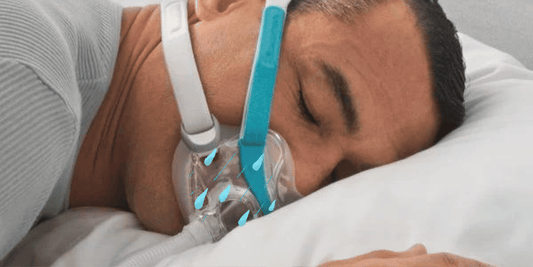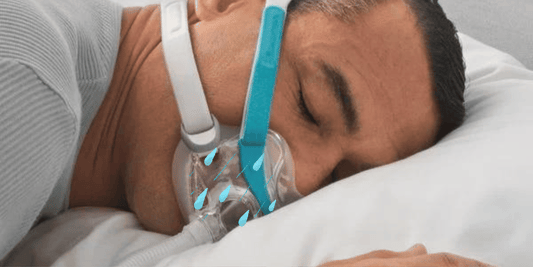
A restful night's sleep might be a luxury that individuals dealing with obstructive sleep apnea (OSA) find elusive. OSA, a sleep-related breathing disorder, manifests through repeated obstructions in the upper airway.
Co Morbidity Explained
OSA is not just “snoring” while sleeping. It is deemed as a serious condition as co morbidities of OSA are possible. Co morbidity refers to a medical condition that is simultaneously yet independently occurs with another medical condition. It can also be used to point out a related medical condition or conditions. Co morbidity may also refer to interactions between the illnesses that could affect the prognosis and course of the diseases.
 Studies on OSA Co Morbidities
Studies on OSA Co Morbidities
According to http://mdnews.com,, recent medical literature and studies done by independent entities concluded that people with undiagnosed and untreated sleep apnoea are more likely to develop co-morbidity in cardiac, immunologic, neurologic and metabolic functions. In the United States, there is evidence that 75% of stroke patients and diabetics, and one-third of patients diagnosed with heart disease have a sleeping disorder.
Studies done by Australia-based Sleep Health Foundation Organisation indicate that patients with OSA are more at risk of developing cardiovascular diseases, diabetes, metabolic syndrome and depression. There are indications that people with untreated OSA are more likely to get involved in vehicular accidents and incidents in the workplace.
Research indicates that children experiencing OSA are at an increased risk of developing Attention Deficit Hyperactivity Disorder (ADHD). ADHD is marked by traits such as inattention, impulsivity, and, in certain instances, hyperactivity. This correlation not only underscores the potential connection between OSA and ADHD but also emphasises the possible impact on both learning and emotional well-being.
Possible Co-occurring illnesses with OSA
Medical consequences of untreated sleep apnoea have been observed and documented in various medical literature over years. These illnesses may or may not be a consequence of OSA as the sleeping disorder could be a symptom of the pertaining health condition. A short list of co morbidities of OSA includes: diabetes (type 2), depression, cardiovascular diseases, hypertension, metabolic syndrome, adult asthma, liver problems and acid reflux.
Cardiovascular diseases include stroke, congestive heart failure, heart valve problems and arrhythmia. Metabolic syndrome is a cluster of conditions wherein high blood sugar level, increased blood pressure, high cholesterol level, and excess body fat around the waist are manifested. These symptoms increase the risk of developing type 2 diabetes, stroke and heart disease.
Medical researchers have concluded that 70% of patients with OSA have systemic hypertension and that OSA increases by 27% the development of coronary artery disease. Patients with OSA are 3 times more likely to develop type 2 diabetes. OSA may also be a symptom of an undiagnosed auto-immune disease.
Other Consequences of Untreated OSA
Untreated OSA is also responsible for low job performance and productivity in adults and poor academic performance in children. Research has highlighted the relationship between increased risk of motor vehicle accidents (MVA) and obstructive sleep apnoea.
According to Austroads:
• People with OSA are two to seven times more prone to MVA
• OSA impairs a person’s driving performance
• People with severe OSA have a higher incidence of MVA than those with mild to moderate OSA
Treatment
Mild OSA may be corrected through behavioural modifications such as proper sleeping position, weight loss, and avoidance of sedatives and alcohol. What about for those with moderate to severe OSA?
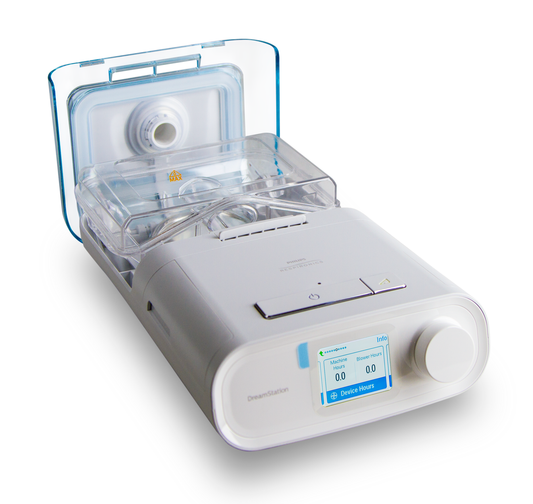
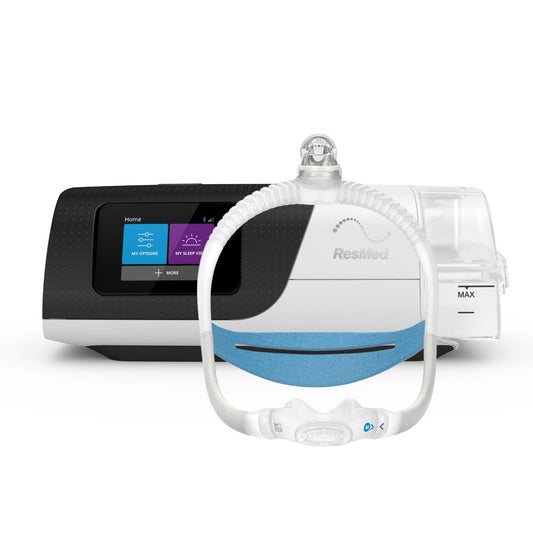
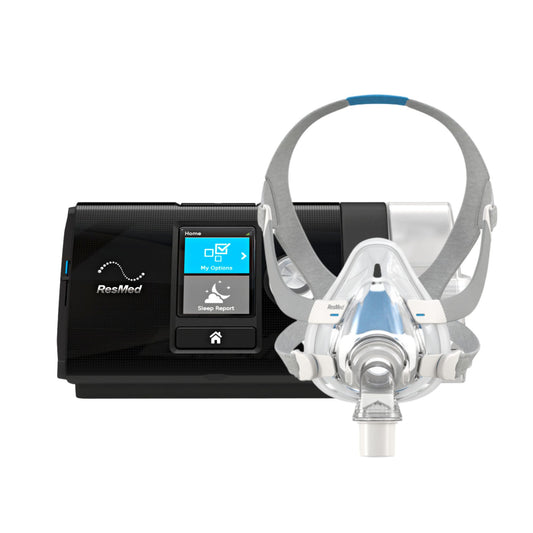
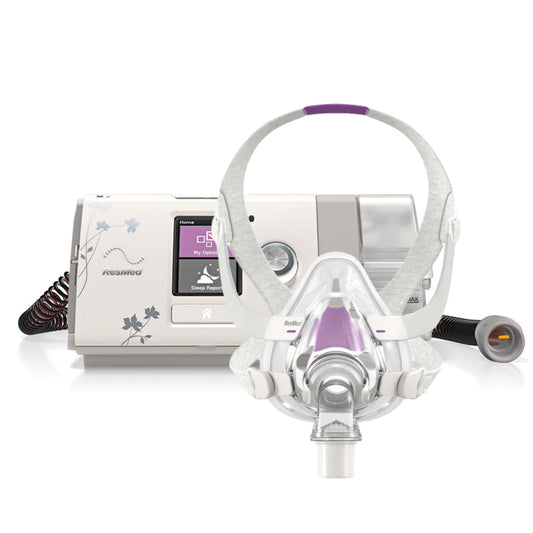
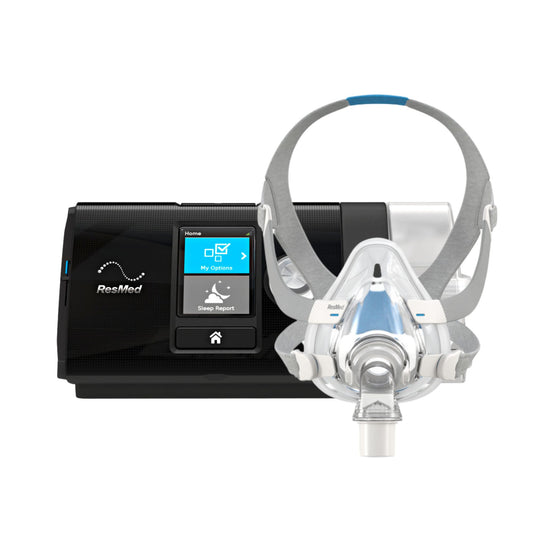
An effective and non-invasive treatment option for patients with different levels of OSA is the use of continuous positive airway pressure or CPAP. The patient is required to wear a facial or nasal mask during sleep as the CPAP acts as a pneumatic stent to ensure a clear airway path.
Find a clinic or call us now for a consultation 1300 750 006.