However, even with the new technology, people still have CPAP therapy side effects. These problems can be prevented if the CPAP user learns about the problems that may occur. Some of the most common side effects of CPAP therapy are: effects on the esophagus; gas in the stomach; congestion and sinus infection; dry mouth; mask discomfort; too much noise; and tendency to pull off the mask while sleeping. Below are two of the side effects.
Effects on the Esophagus
As reported by users, the most common esophagus side effects are acid reflux, vomiting and nausea. These side effects are due to Gastroesophageal Reflux Disease (GORD), where the muscles at the end of the esophagus do not properly close, thereby allowing the content of the stomach to flow into the mouth or throat. Due to the continuous high pressure delivered by CPAP, GORD can be aggravated. This happens when the CPAP high pressure air is swallowed into the esophagus. This opens the muscular valve of the esophagus, allowing the air to flow into the aerophagia (stomach) to flow back from the source. All is not lost though as treating GORD will prevent the flow of air to the user’s stomach, which effectively stops the vomiting and nausea.
Managing the negative consequences is easy enough.
- Try lifting the head and upper body as one sleeps. This can be done by using a sleep wedge or more pillows
- Eat light dinner several hours before going to sleep
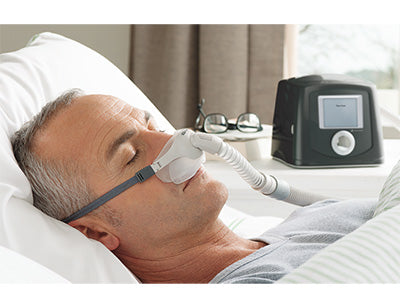
- Try using a nasal or nasal pillow mask as this will stop you taking air in into your stomach
- You can choose to wear a nasal mask or nasal pillows mask instead of a full face mask
- If the CPAP pressure is too high, you can reduce the pressure and then gradually increase the pressure under a doctor’s advice.
- You can try switching to BiPAP
Gas Bloating
Air in the stomach is very uncomfortable and at times quite painful. This condition is called aerophagia and is very common experience for CPAP users. The discomfort usually goes away but for some, it does not if they have GORD. The solution is to switch to a BiPAP machine and make sure that there is no air leaking through the mouth. It is also advisable to switch to either a nasal mask or pillow mask. It will also help if a user trains himself to sleep with his tongue in contact with the back of his front teeth and the mouth’s roof. This will help keep the air in the upper airway and prevent the user to swallow air.
Next we will discuss the other problems and their solutions to side effects of CPAP therapy. Meantime, if you have questions regarding CPAP therapy please call us anytime.
]]>







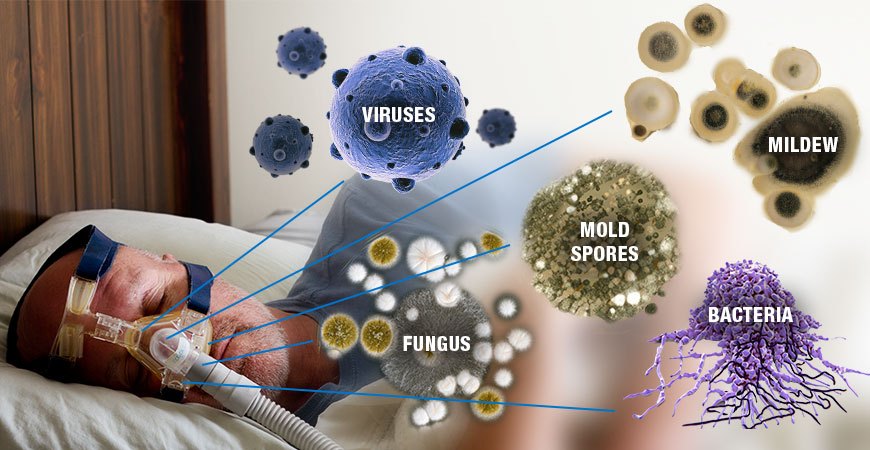





 Sinus Irrigation: One way of getting rid of congestion is by doing sinus irrigation or rinse. Doing this will clear one’s nose of mucus, making it easier for the CPAP user to breathe. Sinus irrigation will also clear the nose of any allergen or germs that could irritate the lining of the nose. It is best to consult with an ENT initially. There are sinus rinse kits available over the counter.
Sinus Irrigation: One way of getting rid of congestion is by doing sinus irrigation or rinse. Doing this will clear one’s nose of mucus, making it easier for the CPAP user to breathe. Sinus irrigation will also clear the nose of any allergen or germs that could irritate the lining of the nose. It is best to consult with an ENT initially. There are sinus rinse kits available over the counter.